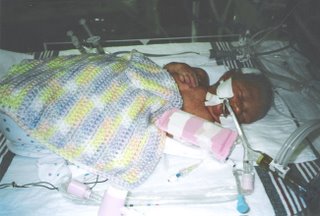
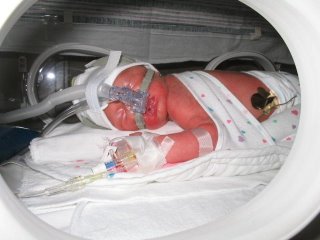
Taegan Sage McFarland was born two months early on 6-3-04, weighing 4lbs. 4oz. via emergency C-section due to a compromised umbilical cord and numerous other contributing factors.
She spent one month in the neonatal intensive care unit on a ventilator, battling pulmonary hypertension, respiratory infection, low blood pressure, patent ductus arteriosus (hole in the heart), poikilothermia (inability to maintain body temperature), apnea, reflux, and jaundice.
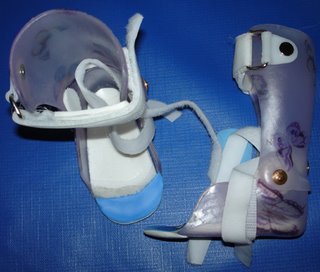
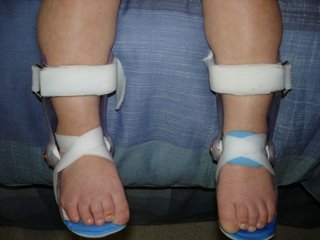
Since her birth, Taegan has struggled to conquer developmental milestones, and often lags behind her peers by 12-15 months. She is significantly speech delayed, having approximately five intelligible words, and uses some simple sign language for basic needs. Taegan has limited use of her legs due to increased muscle tone. She wears ankle foot orthotics (AFO's) on her legs to help with her tone issues.
We live in the small town of Greenwood, about 10 minutes south of Indianapolis. Shortly after Taegan's birth, Shawn began working two jobs in an effort to financially support our family and to keep up with the mounting medical bills. Unfortunately, in January, 2006 we lost our home in part because of the overwhelming medical bills that accrued since the latter part of my pregnancy with Taegan, and the subsequent NICU stay after her birth. We learned that despite having decent medical insurance, you can still walk away with a $30,000+ bill! Also, going from two incomes to one drastically changed things, and it simply became too much.
I was strongly advised by the NICU doctors to keep Taegan out of any type of day-care setting for as long as possible, especially up through her second year of life. This was advised because of the increased risk Taegan runs of catching a potential deadly virus (to preemies and respiratory compromised babies) called Respiratory Syncytial Virus (RSV.) Because of this risk, Taegan received monthly RSV shots at the hospital (approximately $4,500 per shot!) Thankfully, she no longer has to receive these shots, as the risk of developing serious complications from the virus goes down as her age increases.
In August, 2006 Taegan was diagnosed with Cerebral Palsy/Periventricular Leukomalacia/Spastic Diplegia. This diagnosis includes a plethora of possible ailments such as visual problems, hearing problems, seizures, learning disabilities, speech difficulties, sensory processing disorders, musculoskeletal issues and endocrinological concerns, to name a few.
Taegan has been receiving conventional therapies (Occupational, Physical, Speech, Nutritional) since the age of six months. While they play an important role in her development, there are also many non-traditional therapies which are yielding promising results. We'd like to pursue those avenues for Taegan, however, insurance companies do not cover non-traditional therapies and those that are not approved by the FDA for specific diagnoses.
Hyperbaric oxygen treatments (HBOT) are one of these non-FDA approved therapies. HBOT is approved by the FDA for use with wound care patients, however, cerebral palsy is not a recognized diagnosis for the treatment. That does not mean that we cannot pursue this avenue of treatment for our daughter. It simply means we will have to fund these treatments out of pocket. A typical cycle (40 one-hour sessions) of HBOT costs approximately $10,000 here in the United States.
Our hope for Taegan, as it is every parents hope, is for her to be able to live the fullest life possible. For her, unfortunately that also means struggling to overcome physical limitations. Limitations which very well could be lessened with HBOT. We're counting on God's magnificent earth angels (YOU!) to help us realize this hope for our daughter. Thank you for taking the time to read about our daughter and our cause.
Sincerely, Shawn, Michelle and Taegan McFarland
Angels 4 Taegan
520 North State Road 135
Suite M - 147
Greenwood, IN 46142